As outbreaks of COVID-19 occur across the country, hospitals and healthcare systems continue to respond with live-saving resources and heroic measures to treat and care for patients. The response to the pandemic has created significant financial challenges for hospitals and healthcare systems from the effects of COVID-19 testing, treatment, and care. In addition to the cost incurred for caring for COVID-19 patients, hospitals face a 54% drop in patient visits originally from the cancelation of non-emergency and elective procedures. Deferral of procedures is continuing with the fear that one will get infected with the highly transmissible virus simply by going to a hospital for care. As a result, hospitals’ staggering losses in revenue are mounting. According to a new study by Strata Decision Technology, United States (U.S.) hospitals are losing an estimated $60.1 billion a month and facing a 114% increase in uninsured patients from individuals losing employer sponsored insurance.
Our team at Hagerty Consulting is working with hospitals, healthcare systems, and universities across the country to maximize federal and state short-term liquidity funding opportunities and long-term cost recovery. We craft custom cost recovery roadmaps by understanding the unique expenses incurred along with revenue lost to strategically apply the various state and federal programs available to meet the needs of each institution.
Available Federal Funding Opportunities
To help offset lost revenue and costs incurred for testing, treating, and caring for COVID-19 patients, the federal government allocated $175 billion in relief to hospitals. This funding has been allocated through the Health & Human Services (HHS) Provider Relief Fund (PRF) as follows:
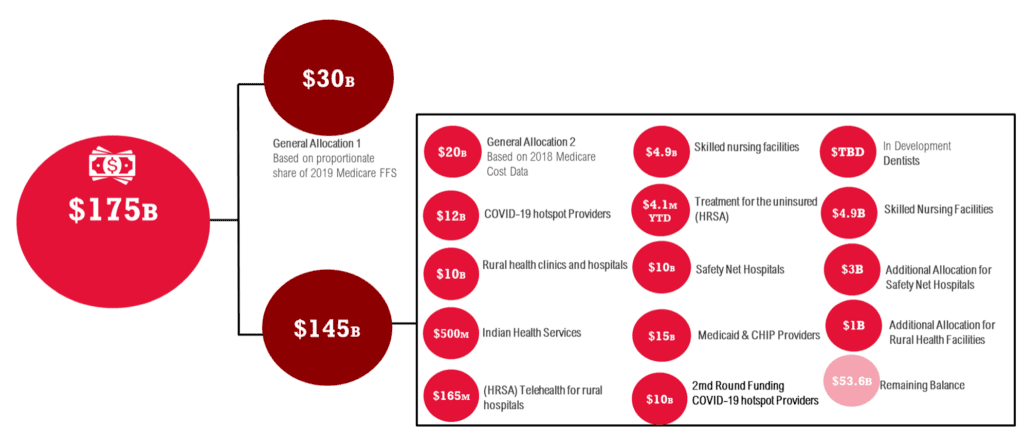
In addition to the $175 billion in relief through the HHS PRF, hospitals are eligible to apply for funding through various other programs, with up to $616 billion in available funding through known allocations and funding streams.
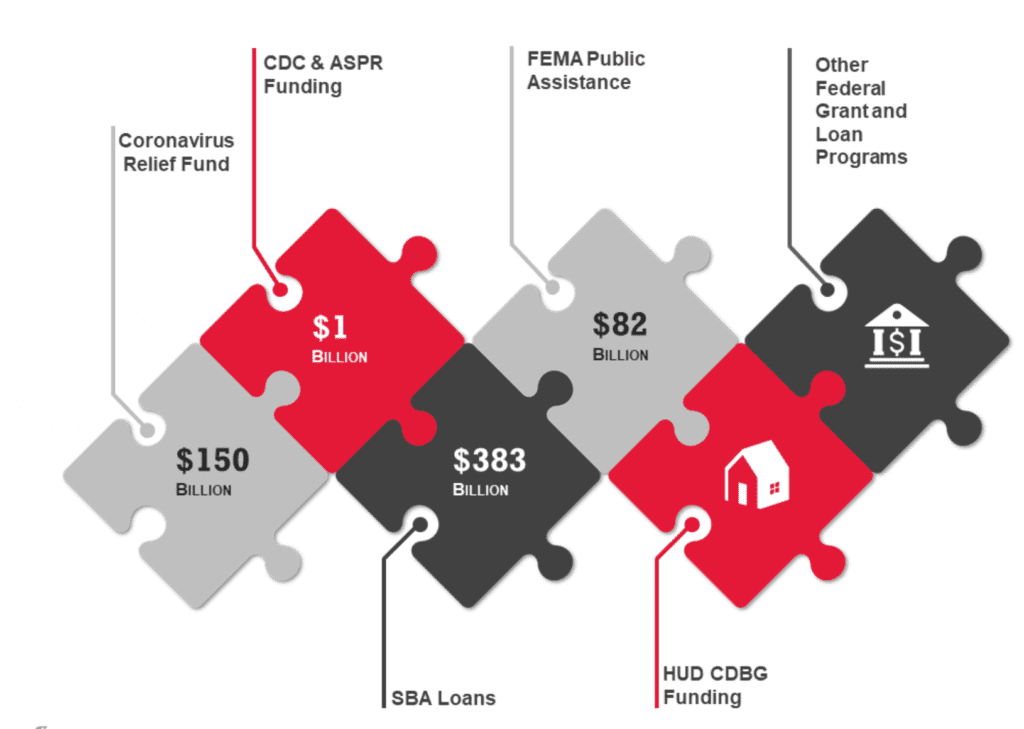
Prospective Federal Funding Opportunities
The U.S. House of Representatives passed the Health and Economic Recovery Omnibus Emergency Solutions (HEROES) Act. The HEROES Act would provide an additional $100 billion appropriation for the PRF along with new provisions for unobligated PRF funding– originally allocated from the Coronavirus Aid, Relief, and Economic Security (CARES) Act and the Paycheck Protection Program and Healthcare Enhancement (PPPHCE) Act — can be distributed and utilized. Currently, the HEROES Act is being considered by the U.S. Senate. If enacted, the law will likely have much needed application-based distributions that will help healthcare providers not only with incurred eligible expenses from caring for COVID-19 patients, but also lost revenue.
On June 12, 2020, the U.S. House of Representatives also introduced the COVID-19 Hospital Forgiveness Act. This Act would facilitate loan forgiveness for hospitals and healthcare providers who applied for and received Medicare accelerated and advanced payments. Without the COVID-19 Hospital Forgiveness Act, the $40.4 billion total loan amount will begin to be repaid by providers who received loans. These payments would begin in August of 2020 through the offset of additional Medicare payments.
Hospitals are facing a severe economic crisis. Our team at Hagerty Consulting offers real-time guidance to navigate the complex and dynamic disaster recovery funding available, including programs through the CARES Act, the Federal Emergency Management Agency (FEMA) Public Assistance (PA) Program, the Coronavirus Relief Fund (CRF), and other federal and state grants available to support recovery. Our diverse team of policy, healthcare, and financial management experts work with our hospital and healthcare system clients from start to finish in the complex application process to seek and maximize federal and state reimbursement for COVID-19 incurred costs and revenue loss. We emphasize timeliness and efficiency balanced with regulatory compliance to position organizations to capture eligible costs for reimbursement without experiencing de-obligation in the future.
The COVID-19 emergency is an unprecedented public health and economic challenge. The robust federal funding provided so far has been essential for hospitals to be able to continue to deliver much needed medical care. Going forward, additional federal funding will be necessary to properly outfit our public health infrastructure and prepare hospitals that are caring for the sickest of COVID-19 patients while advancing financial recovery in the midst of a prolonged emergency response.
Jeff Bokser is Hagerty Consulting’s Vice President of Healthcare Programs with strategic expertise in all aspects of healthcare operations, finance, crisis management, and recovery. Jeff has over 20 years of experience as a senior leader at NewYork-Presbyterian and Yale New Haven Health. He advanced performance and increased revenue in clinical and nonclinical settings and led innovation in daily operations and care delivery processes. Jeff is nationally recognized in the healthcare sector for his transformational leadership in the areas of emergency and crisis management; security and safety; pandemic and surge planning; and business continuity. Jeff was the system-level executive responsible for Emergency Medical Services, Emergency Management, Business Continuity, Crisis Management, Safety, Security, and Regulatory Compliance for the entire continuum of the NewYork-Presbyterian Hospital & Healthcare System enterprise. He served as Incident Commander guiding 40,000+ employees through numerous internal and external emergency response and recovery operations including Hurricane Sandy, Ebola, H1N1, and 9/11.